Whether you've been scouring the keto subreddits, watching your favorite YouTube keto pros, or reading the countless keto forums, it's likely that you've come across the term GKI, which stands for the Glucose Ketone Index. This may have left you wondering, "What exactly is the GKI?"
QUICK REFERENCE
- Understanding What GKI Is All About
- Necessary Tools
- How to Calculate Your GKI
- What Your GKI Number Means
- Understanding GKI Ranges
- How to Test Your GKI (Step-by-Step)
- Ways to Use GKI Tracking
- Using GKI to Guide Your Approach
- What Impacts Your GKI
- How to Improve Your GKI (If It's Higher Than Expected)
- Common GKI Mistakes to Avoid
- Putting It All Together
- Discussion
At first glance, it seems like just another metric to track. In practice, though, the GKI is one of the most valuable tools for understanding how your body responds to a ketogenic diet.
In this guide, you'll learn what the GKI is, how to calculate it, how to interpret your numbers, and most importantly, how to use it to make informed, personalized decisions about your nutrition and lifestyle.
Understanding What GKI Is All About
The GKI was developed by Dr. Thomas Seyfried while working with brain tumor patients. It was created to track and manage a patient's metabolic state for better brain tumor management. Essentially, his work involved using the GKI to optimize the metabolic state that most effectively halts brain tumor growth.
In simplest terms, the GKI is an equation that tracks the ratio of blood glucose to ketones as a single value. In this format, it becomes an easy biomarker for tracking the level of ketosis you're in and keeping tabs on your overall metabolic health. (1)
As we all have bio-individuality, what works for one will not necessarily work for another. The GKI provides a stable metric to help you find what works best for your body.
Necessary Tools
To measure your GKI, you'll need access to a glucose and ketone testing method. The most common option is a blood meter, like the KetoMojo testing meter, that uses a finger prick, test strips, and a handheld device. (2)
Some individuals also explore breath-based ketone meters as a lower-cost, non-invasive alternative. While these may not always provide identical readings, they can offer useful trend data over time.
Whichever method you choose, consistency is most important. Using the same device under similar conditions will give you the most reliable insights.
How to Calculate Your GKI
No need to stress about the numbers because you'll find plenty of online calculators that will run the computation for you. But, for those of you who like to go into things with full knowledge, here's the equation that's used to determine your GKI.
[Glucose Reading (mg/dL) ÷ 18] ÷ Ketone Reading (mmol/L) = Glucose Ketone Index
An online calculator or app requires you to plug in your readings, and then it does the work for you. Then all you'll need to do is match up your GKI number to your target and assess from there.
What Your GKI Number Means
Once you've calculated your GKI, the next step is understanding what that number is telling you. Think of your GKI as a snapshot of your metabolic state at a given moment.
Rather than looking at glucose or ketones in isolation, the GKI combines them into a single, more meaningful metric, making it easier to understand where you fall along the spectrum, from little to no ketosis to deeper, more therapeutic levels.
Your ideal range will depend on your goals. For general metabolic health or weight management, moderate levels of ketosis may be appropriate. In more targeted therapeutic settings, deeper levels of ketosis may be explored under clinical guidance. (3)
The ranges below provide a practical framework for interpreting your results.
Understanding GKI Ranges
The following ranges offer a simplified way to interpret your GKI and understand how deeply you're in ketosis. These are general guidelines and should always be interpreted within the context of your individual goals and clinical situation.
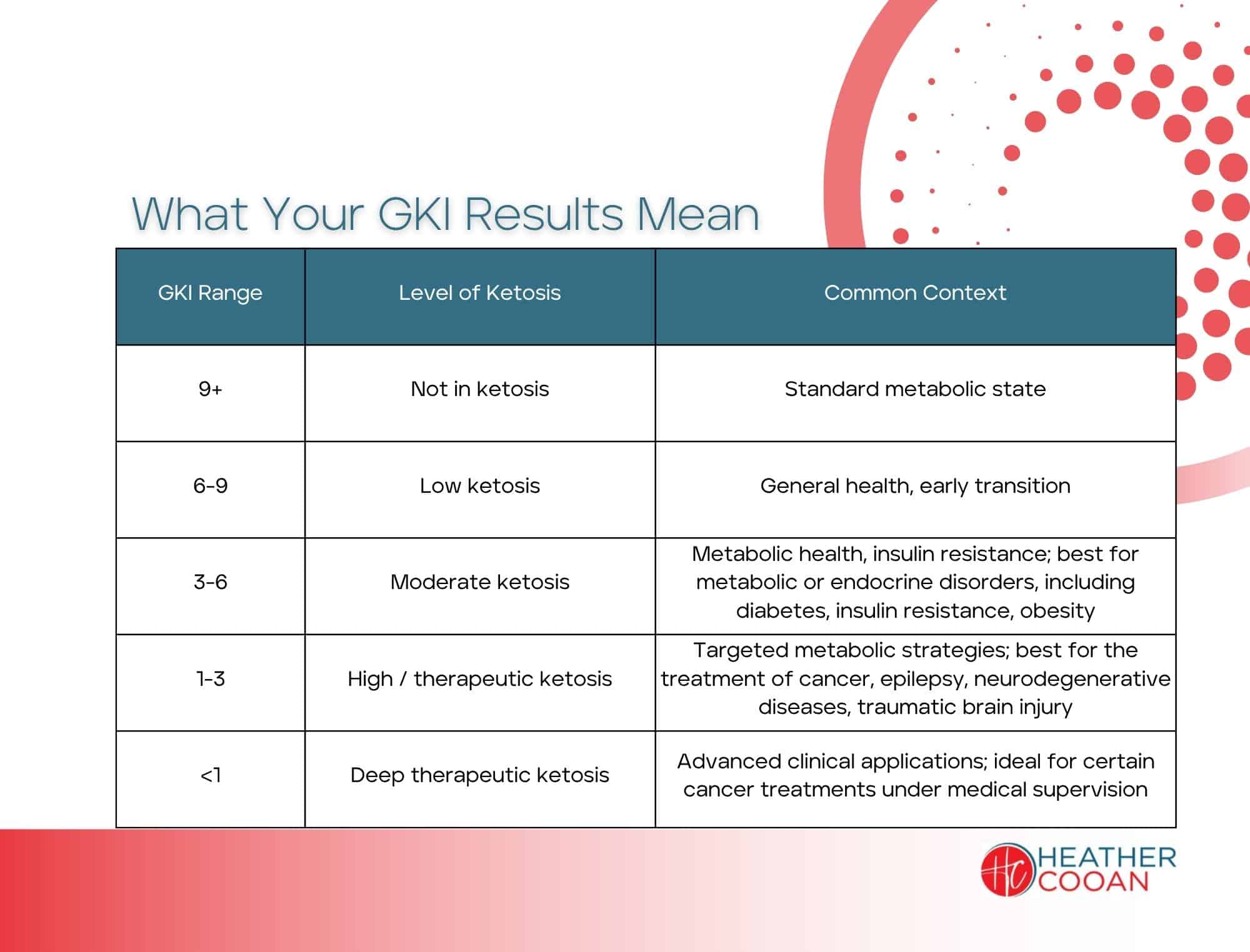
Lower GKI values reflect a metabolic state in which ketones are more dominant than glucose. These deeper levels are typically more structured and pursued with professional guidance in clinical settings.
How to Test Your GKI (Step-by-Step)
To get the most meaningful data from your GKI, consistency and context matter.
Here's a simple framework to follow:
Step One: Choose a consistent testing time
- First thing in the morning (fasted)
- Or a set number of hours after eating
Step Two: Measure both glucose and ketones
- Use a blood glucose/ketone meter
- Record both values before calculating GKI
Step Three: Start with 1-2 readings per day
- Morning baseline
- Optional second reading later in the day
Step Four: Track patterns over time
- Look for trends - patterns, not perfection!
- Compare readings taken under similar conditions
Ways to Use GKI Tracking
There are several ways to use GKI depending on your goals:
Daily Tracking
- Take one consistent reading per day
- Helps establish baseline trends
Full-Day Tracking (Short-Term)
- Test every 2-3 hours for 1-2 days
- Helps identify patterns and responses
Food and Activity Testing
- Measure before and after meals or activities
- Helps identify personal sensitivities
These approaches allow you to move from general guidelines to personalized insights.
Using GKI to Guide Your Approach
Once you understand what your GKI number represents, it becomes a powerful tool for personalization. Rather than simply following general keto guidelines, tracking your GKI allows you to see how your body responds in real time, and that gives you insight into what's actually working for you.
This is where GKI becomes especially valuable. Two people can follow the same ketogenic diet and experience very different results depending on factors like carbohydrate tolerance, protein intake, stress levels, sleep quality, and overall metabolic health. Your GKI helps clarify those variables.
For some, the goal may be maintaining a moderate level of ketosis to support metabolic health or weight management. For those in more therapeutic contexts, there may be a need to reach deeper levels of ketosis consistently. In these cases, GKI tracking can help guide more precise adjustments and help you monitor your progress over time.
Tracking your personal experience can be very powerful because patterns begin to emerge when you consistently measure your GKI. You can start to identify how specific foods, lifestyle factors, and even stress or sleep impact your numbers-allowing you to move from guessing to a more data-informed approach.
What Impacts Your GKI
Dietary Factors (Primary Drivers)
Carbohydrate Intake (Quantity)
It will come as no surprise that the amount of carbohydrate you eat has a direct effect on your GKI. The more carbs you consume, the higher your blood glucose is likely to be, which can push your GKI up even if ketones are present. (4) Reducing carbs generally helps your body switch to fat and ketones for fuel, lowering your GKI over time.
Your personal carbohydrate threshold, or the amount at which your body starts producing significant ketones, can vary. Some people enter ketosis at fewer than 20 grams of net carbs per day, while others may tolerate slightly higher amounts if the carbs are from whole foods. Monitoring your GKI alongside carb intake helps you find the level that works best for you.
It's also worth noting that periods of transition or adaptation can temporarily elevate glucose even with restricted carbs, which is a normal response as your metabolism adjusts to burning fat and ketones.
Carbohydrate Quality
Not all carbs affect your GKI equally. Processed and refined carbohydrates, such as prepackaged sweets, breads, and snack foods, can spike blood glucose more dramatically than whole-food sources like leafy greens, cruciferous vegetables, or berries.
Even small amounts of highly processed carbs can temporarily raise glucose, lowering your ketone levels and increasing your GKI. In contrast, high-fiber, minimally processed carbs often have a smaller impact, allowing you to maintain lower GKI readings while still getting important nutrients. (5)
Paying attention to carbohydrate quality while tracking your GKI can reveal which foods your body tolerates well and which disrupt ketosis.
Protein Intake
Too much protein can influence your GKI. When protein intake exceeds immediate energy needs, your liver can convert some amino acids into glucose through a process called gluconeogenesis. (6) This can raise blood glucose and temporarily increase your GKI, even if you're in ketosis.
Your sensitivity to protein varies. Some people can consume higher amounts without significant changes in GKI, while others experience more pronounced effects. Tracking your GKI alongside protein intake allows you to fine-tune amounts to support muscle maintenance without inadvertently disrupting therapeutic ketosis.
This is particularly important for individuals pursuing deeper, therapeutic ketosis for clinical purposes, because protein management can help maintain the desired GKI range.
Meal Timing and Frequency
When and how often you eat can affect your GKI just as much as what you eat. Longer periods without food, such as intermittent or prolonged fasting, can increase ketone production and lower your GKI. Frequent meals or snacks, especially those with carbohydrates, may keep glucose higher and ketones lower.
Your GKI can also help you understand how meal timing interacts with your metabolism. (7) For example, you may notice that ketones are higher and glucose is lower after a prolonged fast. Still, during periods of stress or hormonal changes, readings may fluctuate even with consistent fasting practices.
For those using ketogenic approaches therapeutically, structured timing and intentional fasting windows can be powerful tools, but GKI tracking ensures adjustments are based on actual metabolic responses rather than guesswork.
Metabolic and Lifestyle Factors
Physical Activity and Exercise
Anything that significantly influences glucose and ketone metabolism will also influence your GKI. During and after exercise, the body shifts fuel utilization to meet increased energy demands. Ketones provide an alternative source of energy when carbohydrates are low, and muscles that are well‑adapted to burning fat and ketones may use them more efficiently, helping your body recover from exercise and bringing blood glucose back to baseline more smoothly.
Exercise may also acutely increase blood glucose, particularly in some high-intensity contexts or if hepatic glucose output increases to support working muscles. At the same time, ketone concentrations may decline as they're oxidized for fuel. (8)
Over time, consistent activity and exercise tend to improve metabolic flexibility, decreasing resting glucose and supporting more stable ketone production. Using GKI alongside activity tracking can help clarify whether exercise is shifting your metabolic response in expected ways or if adjustments to training intensity or timing may be beneficial.
Stress and Nervous System Load
Both physiological and psychological stress activate the sympathetic nervous system and the hypothalamic‑pituitary‑adrenal (HPA) axis, thereby increasing circulating stress hormones, including cortisol and catecholamines. These shifts promote gluconeogenesis and reduce insulin sensitivity, which can elevate blood glucose levels independent of dietary intake.
Chronic or repeated stress responses amplify inflammatory processes that compromise insulin signaling and glucose regulation. (9) From a GKI perspective, this means that periods of persistent stress may lead to higher glucose readings and suppressed ketogenesis, resulting in a temporarily higher GKI even when diet and fasting protocols remain consistent.
Understanding how stress affects your GKI and using stress management practices can help you support your overall metabolic balance.
Sleep Quality and Recovery
Quality sleep is another key component of glucose regulation and metabolic homeostasis. (10) During deep sleep, insulin sensitivity tends to be higher and stress hormone levels lower. When normal sleep is disrupted, sympathetic nervous system activity increases, elevating catecholamines and impairing glucose metabolism.
Studies show that fragmented or insufficient sleep patterns can decrease insulin sensitivity and impair glycemic control. These effects can lead to higher fasting glucose and potentially weakened ketone production. From a clinical perspective, optimizing sleep can be a foundational metabolic intervention.
Illness and Inflammation
When you're dealing with an acute illness, like a cold or flu, your GKI may rise even while fasting. This is because your body shifts energy priorities to support your immune system. (11) Cortisol and other stress hormones push your body to rely more on glucose for quick energy, causing ketone production to drop temporarily. This is a normal, adaptive response, and is not a sign that your keto plan isn't working.
If you're a cancer patient or dealing with another major illness, these changes can be even more noticeable. Since your body is already under metabolic stress from the disease or other treatments, an acute illness can further increase glucose availability while lowering ketones. So even when you're following a therapeutic ketogenic diet carefully, it's common to see a higher GKI during illness.
Chronic inflammation can also affect your GKI. Persistent inflammation reduces insulin sensitivity, keeping blood sugar elevated and lowering ketone production.
Hormonal Fluctuations and Your Menstrual Cycle
For women, hormonal shifts throughout the menstrual cycle can have a noticeable impact on blood glucose, ketone levels, and, of course, your GKI.
According to diabetes research, as well as anecdotal and clinical observations, women who track their GKI report that blood glucose runs higher and ketones lower than usual right before the menstrual cycle begins, and this remains consistent even during extended fasting. (12)
In other words, it's not uncommon to see higher blood glucose and lower ketone readings in the days leading up to and during menstruation, even when diet, fasting, and lifestyle habits remain consistent. This can result in a temporarily elevated GKI that may feel confusing if you're not expecting it.
The key takeaway here is that these shifts are physiological, not a sign that something is "going wrong." Rather than reacting by over-restricting or making drastic changes, it's often more helpful to zoom out, track patterns over time, and interpret your GKI within the broader context of your body's natural rhythms.
Advanced Physiological Factors (Less Common Drivers)
Adaptive Glucose Sparing
If you've been following a keto diet for a longer period of time, you may notice that your fasting blood glucose is slightly higher than expected, even when you're doing everything "right." This is often referred to as adaptive glucose sparing. (13)
When your body becomes highly efficient at using fat and ketones for fuel, some tissues (like muscles) start relying less on glucose. As a result, glucose can remain in the bloodstream rather than being taken up as quickly, leading to slightly elevated blood sugar levels and a higher GKI.
While this can feel frustrating, it's often a normal adaptation rather than a sign of poor metabolic health. Tracking your GKI over time can help you determine whether this is a stable pattern for you or warrants further investigation in a clinical context.
Individual Metabolic Variability
No two people will have the same GKI response, even when following similar diets. A range of factors, including genetics, metabolic health, hormone balance, activity level, and medical history, influence your metabolism. (14)
You may find that certain foods, protein levels, or fasting strategies produce very different results for you compared to someone else. This is why tracking your GKI can be so valuable. Understanding how your body uniquely responds to different variables allows you to move beyond general guidelines and into true individuation.
Over time, your own patterns begin to emerge, and you begin to notice specific foods, stress levels, or routines that consistently raise or lower your GKI. These insights can then be used to guide the most personalized and effective decisions for you, rather than relying on a one-size-fits-all approach.
Gut and Digestive Factors
Your digestive health can also influence your GKI, sometimes in less obvious ways. How well you break down and absorb food affects how quickly nutrients enter your bloodstream, which in turn affects both glucose and ketone levels.
When digestion is slow, glucose may enter the bloodstream more gradually or later than expected, leading to delayed or unpredictable changes in your GKI. Rapid digestion or impaired gut health may lead to sharper glucose responses.
Gut health, inflammation, and the composition of your microbiome have all been shown to influence glucose metabolism and insulin sensitivity. (15) Paying attention to how your body responds, especially if your readings feel inconsistent, can help you identify whether digestive factors may be playing a role.
Testing Context Matters
Fasted vs Fed State
Whether you measure your GKI in a fasted or fed state can significantly influence your results. When you haven't eaten for several hours, your body is more likely to rely on stored fat for fuel, which can increase ketone production and lower your GKI. (16)
After eating a meal that contains carbohydrates or protein, blood glucose may rise, and ketone levels may temporarily drop. This can lead to a higher GKI reading, even if your overall metabolic state is still aligned with your goals.
For this reason, consistency matters. Tracking your GKI under similar conditions (for example, first thing in the morning or a set number of hours after eating) can help you better understand your patterns and avoid misinterpreting normal fluctuations.
Time of Day
Your GKI can naturally vary depending on the time of day you measure it. Many people experience higher blood glucose levels in the morning due to the "dawn phenomenon," in which hormones signal the liver to release glucose to prepare the body for waking. (17)
As the day goes on, glucose levels stabilize, and ketone production typically increases, especially if meals are spaced out and carbs are kept low. This means your GKI in the afternoon or evening may look very different from your morning reading, even if nothing else has changed.
Understanding these natural rhythms can help you interpret your results more accurately. Rather than focusing on a single reading, it's much more helpful to compare values taken at the same time of day and look for trends over time.
Acute vs Long-Term Trends
A single GKI reading only tells you what's happening at that moment. Day-to-day fluctuations are normal and can be influenced by everything from stress and sleep to activity and hydration.
What matters most is the pattern over time. Consistently tracking your GKI allows you to see trends. Are your numbers generally moving in the direction you want? Are they staying stable? Are they being affected by certain habits or conditions?
Asking yourself these questions and looking at long-term trends can help you avoid overreacting to short-term changes. A higher reading on one day doesn't necessarily mean something's off. Think of it as an opportunity to step back, look at the bigger picture, and make informed adjustments if needed. Patterns over perfection!
How to Improve Your GKI (If It's Higher Than Expected)
If your GKI is higher than your target range, it doesn't necessarily mean something's wrong. Instead, it's an opportunity to look at key variables that may be influencing your results.
Start with nutrition:
- Review carbohydrate intake (quantity and quality)
- Evaluate protein intake
Then consider lifestyle factors:
- Stress levels
- Sleep quality
- Physical activity
Next, look at the testing context:
- Were you fasted or fed?
- Time of day?
- Recent illness or hormonal changes?
Finally, zoom out and assess trends over time rather than reacting to a single reading.
Small, consistent adjustments that are guided by your data will prove more effective than drastic changes.
Common GKI Mistakes to Avoid
When using GKI, a few common pitfalls can lead to confusion:
- Testing at inconsistent times
- Comparing fasted and fed readings directly
- Overreacting to a single data point
- Ignoring factors like stress, sleep, or illness
- Assuming lower is always better
Understanding these variables helps you interpret your numbers more accurately and avoid unnecessary adjustments.
Putting It All Together
Your GKI isn't just a number. It's a reflection of how your body is responding in real time.
When interpreted within the right context, it becomes a powerful tool for personalization and helping you understand how nutrition, lifestyle, and physiology interact in your body.
Don't aim for perfection, because the goal is awareness. By tracking patterns, adjusting thoughtfully, and staying consistent, you can use your GKI to guide a more informed, responsive, and sustainable approach to your keto diet and your health.
REFERENCES:
- Meidenbauer JJ, Mukherjee P, Seyfried TN. The glucose ketone index calculator: a simple tool to monitor therapeutic efficacy for metabolic management of brain cancer. Nutr Metab (Lond). 2015;12:12.
- KetoMojo. Glucose Ketone Index. Accessed June 22, 2020. Available from: https://keto-mojo.com/glucose-ketone-index-gki/
- Paoli A, Rubini A, Volek JS, Grimaldi KA. Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets. Eur J Clin Nutr. 2013 Aug;67(8):789-96. doi: 10.1038/ejcn.2013.116. Erratum in: Eur J Clin Nutr. 2014 May;68(5):641.
- Biyikoglu H, Robertson MD, Collins AL. Isolating the acute metabolic effects of carbohydrate restriction on postprandial metabolism with or without energy restriction: a crossover study. Eur J Nutr. 2025 Mar 20;64(3):133. doi: 10.1007/s00394-025-03646-5.
- Bian L, Yang C, Jin Y, Wang H, Zhu M, Xu J, et al. Association between carbohydrate quality and glycemic control in individuals with type 1 diabetes: A cross-sectional and meal-based analysis. PLoS One. 2026 Feb 2;21(2):e0341915. doi: 10.1371/journal.pone.0341915.
- Clina JG, Sayer RD, Pan Z, Cohen CW, McDermott MT, Catenacci VA, et al. High- and normal-protein diets improve body composition and glucose control in adults with type 2 diabetes: a randomized trial. Obesity (Silver Spring). 2023 Aug;31(8):2021-2030. doi: 10.1002/oby.23815.
- Ali M, Reutrakul S, Petersen G, Knutson KL. Associations between Timing and Duration of Eating and Glucose Metabolism: A Nationally Representative Study in the U.S. Nutrients. 2023 Feb 1;15(3):729. doi: 10.3390/nu15030729.
- Evans M, Cogan KE, Egan B. Metabolism of ketone bodies during exercise and training: physiological basis for exogenous supplementation. J Physiol. 2017 May 1;595(9):2857-2871. doi: 10.1113/JP273185.
- Yaribeygi H, Maleki M, Butler AE, Jamialahmadi T, Sahebkar A. Molecular mechanisms linking stress and insulin resistance. EXCLI J. 2022 Jan 24;21:317-334. doi: 10.17179/excli2021-4382.
- Briançon-Marjollet A, Weiszenstein M, Henri M, Thomas A, Godin-Ribuot D, Polak J. The impact of sleep disorders on glucose metabolism: endocrine and molecular mechanisms. Diabetol Metab Syndr. 2015 Mar 24;7:25. doi: 10.1186/s13098-015-0018-3.
- Mottale R, Dupuis C, Szklarzewska S, Preiser JC. The metabolic response to stress in critical illness: updated review on the pathophysiological mechanisms, consequences, and therapeutic implications. Ann Intensive Care. 2025 Oct 27;15(1):174. doi: 10.1186/s13613-025-01588-z.
- Gamarra E, Trimboli P. Menstrual Cycle, Glucose Control and Insulin Sensitivity in Type 1 Diabetes: A Systematic Review. J Pers Med. 2023 Feb 20;13(2):374. doi: 10.3390/jpm13020374.
- Zilberter Y, Zilberter T. Glucose-Sparing Action of Ketones Boosts Functions Exclusive to Glucose in the Brain. eNeuro. 2020 Nov 9;7(6):ENEURO.0303-20.2020. doi: 10.1523/ENEURO.0303-20.2020.
- Zeevi D, Korem T, Zmora N, Israeli D, Rothschild D, Weinberger A, et al. Personalized Nutrition by Prediction of Glycemic Responses. Cell. 2015 Nov 19;163(5):1079-1094. doi: 10.1016/j.cell.2015.11.001.
- Canfora EE, Meex RCR, Venema K, Blaak EE. Gut microbial metabolites in obesity, NAFLD and T2DM. Nat Rev Endocrinol. 2019 May;15(5):261-273. doi: 10.1038/s41574-019-0156-z.
- Vasim I, Majeed CN, DeBoer MD. Intermittent Fasting and Metabolic Health. Nutrients. 2022 Jan 31;14(3):631. doi: 10.3390/nu14030631.
- American Diabetes Association. High morning blood glucose. Accessed March 13, 2026. https://diabetes.org/living-with-diabetes/high-morning-blood-glucose






Frank Anthony Brennan says
Is the Glucose in the GKI, Glucose oxidase (GOD) or Glucose dehydrogenase (GDH)?
Heather Cooan, MBA, NTP, FDN-P, ONC says
It's blood glucose as measured with a glucometer.